My daughter Jessica was born with a congenital heart defect (CHD) called hypoplastic left heart syndrome (HLHS). This is a complex CHD where the left side of the heart doesn’t form correctly. Basically this means that Jessica only has half a working heart. Babies born with HLHS need to have heart surgery in order to survive. Jessica had her first operation before she was born. Since birth, she has had four more heart operations, plus several cardiac catheter procedures. This is the story of Jessica’s handmade heart.
The normal heart
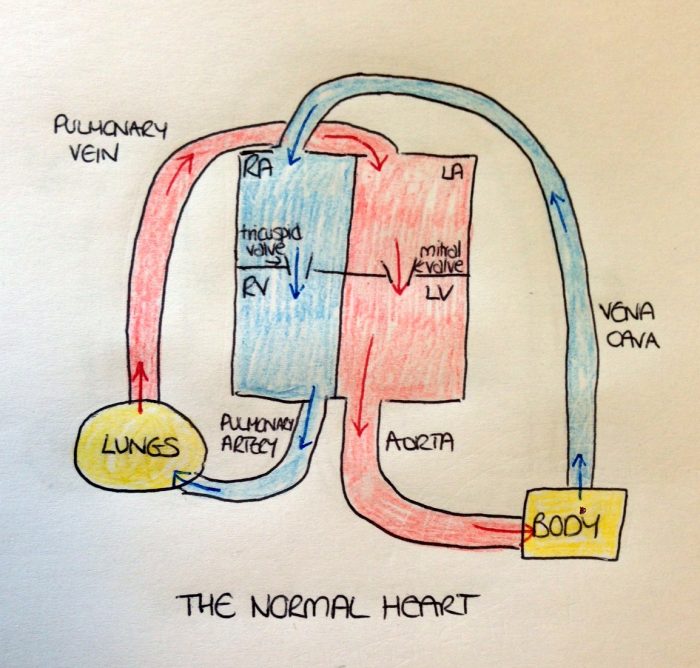
To explain more about Jessica’s special heart, I need firstly to explain how the normal heart works. The picture below is a very simplified diagram representing the normal circulation.
In the normal heart, oxygen-rich, or oxygenated, blood enters the left atrium of the heart via the pulmonary vein. It is pumped through the mitral valve into the left ventricle and then pumped into the aorta where it travels to the body. The blood leaving the body is known as deoxygenated blood (the oxygen having been used by the body). This blood returns to the right side of the heart via the vena cava, entering the right atrium where it is pumped via the tricuspid valve into the right ventricle. It is then pumped from the right ventricle into the pulmonary artery where it travels to the lungs to collect oxygen. The oxygenated blood now leaves the lungs via the pulmonary vein and travels back to the heart and the process begins again.
The HLHS heart
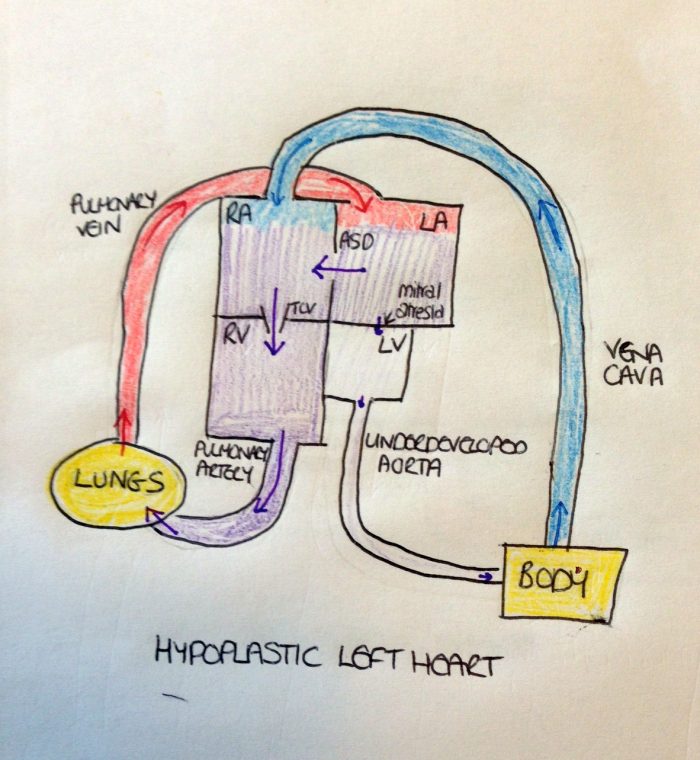
With HLHS, the mitral valve is blocked. This is known as mitral atresia. This blockage prevents the oxygenated blood getting to the left ventricle. However, an atrial septal defect (ASD) (a hole between the top two chambers of the heart) usually forms to allow the blood from the left atrium to pass into the right atrium where it mixes with the deoxygenated blood before passing into the right ventricle, through the pulmonary artery and back to the lungs. Because very little blood is able to get into the left ventricle and into the aorta, the aorta is underdeveloped.
The fetal heart
The circulation of a baby in the womb is a little different from the normal circulation. In the womb, the baby has a duct called the ductus arteriosus which connects the pulmonary artery and the aorta. This duct allows blood to pass into the aorta and on to the body. There is also a hole between the top two chambers (the atria) called the foramen ovale. This allows blood to pass between the two atria. The ductus arteriosus and the foramen ovale both close a few days after birth. The fetal circulation helps to keep babies born with HLHS alive. Unless surgery is carried out soon after birth, a baby born with HLHS will die.
Jessica’s heart
In Jessica’s case, there was an added complication known as a restrictive atrial septum. This meant that the hole between the top two chambers of her heart was very small and was quite likely to close soon after birth. Before birth this was less of a concern because the foramen ovale allowed blood to travel between the top two chambers. Once this hole closed there would have been nowhere for the blood to go once it entered the left atrium.
Jessica also has a ventricular septal defect (VSD) which is a hole between the bottom two chambers. This allowed some blood to pass into the left ventricle and out through the aorta so her left ventricle was not quite as underdeveloped as in many cases of HLHS.
Jessica’s handmade heart: surgeries
Because of her restrictive atrial septum, Jessica’s prognosis was particularly poor. We were very lucky to be offered fetal surgery to enlarge her atrial septal defect and improve the blood flow between the top two chambers of the heart. After she was born, she needed a further procedure to widen this hole once more and to create a stent between her aorta and pulmonary artery, effectively recreating the fetal circulation in order to allow her time to grow before her next heart surgery.
Jessica’s heart cannot be fixed but through a series of operations, the surgical team will re-plumb the blood vessels around her heart so that the right side of her heart does all the work (meaning that she effectively has half a working heart). The blood will be pumped from the right ventricle around the body and then the blood will return to the lungs under its own pressure (rather than being pumped back through the heart) where it will collect oxygen and then return to the heart before being pumped back around the body. This is usually done as a series of three operations.
Jessica has had the first two of these operations, which are called the Norwood and Glenn procedures. She also had two operations before her Norwood procedure, which collectively are known as the hybrid procedure. The final operation is called the Fontan procedure. This is expected to take place at about the age of five.
The future
About thirty years ago, there was no treatment (other than heart transplant) for HLHS and so life expectancy is unknown. We were told when Jessica was first diagnosed at the 20 week scan, that there was a 50% chance of her living to the age of five. If she made it that far, she would have a good chance of living into her teens and early adulthood. Beyond that, we don’t know. Later, when it became apparent that Jessica’s anatomy was more complex, we were told that she was unlikely to be suitable for surgery at all and that compassionate care (making her comfortable until she passed away) would be offered instead (we had declined the third option of termination). We are hugely grateful for being given the chance for fetal surgery which gave Jessica the option of post-birth surgery and helped her to get here today.
As for the future, we don’t know. Naturally we are anxious about the next procedure, but we live very much day to day and enjoy the moments. It has been a huge blessing to be able to watch Jessica grow and develop. We thank God for every day that we have had with her so far. At the start of our journey we would hardly have dared dream that we’d make it this far.





Thank you for sharing yours and Jessica’s story. I was in tears reading it. I cannot imagine how difficult things must be and can’t imagine how hard it must be to watch your baby go through operations like that.
Modern medicine is amazing, and you and Jessica are amazing too.
She is an absolute cutie!
Thank you – modern medicine is definitely amazing – we are very blessed to have Jessica here with us and hard as the journey has been at times, I would walk every step of it again just to be where we are now 🙂
I cannot even begin to imagine what you and Jessica have been through, and do live with every single day. She’s a gorgeous, happy girl, and it’s a pleasure to get to ‘know’ her via your blog and I’ll continue to follow, of course, to see Jessica fight her way through the next stage and come out smiling xx
Thanks Jocelyn – it is just normal life to us now and of course it can be tough at times but seeing how well Jessica has come on and knowing how very lucky we have been, it is all worth it x
As strong and courageous as ever, Jessica is a blessing and she could not have had more caring and courageous parents you deserve each other, sending love as always Pippa xxx
Aw thank you so much Pippa – I don’t always feel strong or courageous but I know how lucky we are to be blessed with both our beautiful girls. Lots of love to you too xx
Thank you for sharing more details of Jessica’s heart condition. I cannot imagine how hard this must be for you, but it is wonderful getting to know you both through your blog x
Thanks Sara – it is just normal life for us most of the time – we try not to think too much about the scary stuff, it’s just such a huge blessing being able to see Jessica grow and develop 🙂
This is a really informative post, hun. Every time I think about you, I cannot help thinking about how much you and Jessica have had to go through. xxx
Thank you Mel – it helped me understand more about the technical details when I decided to draw it out myself – even after more than three years, I still don’t think I’ve quite got my head around the finer details. I keep seeing lots of stuff coming up on my timehop at the moment from when Jessica was a newborn – amazing to see her now and see how far she has come, we have been so very lucky 🙂
What an utterly incredible little girl you have, and this post has really made me think. Thank you #sharewithme
Thank you – she is my inspiration and I am so very lucky to be her mummy 🙂
It was really interesting to read about Jessica, I’d never heard of her condition before. I’m so glad things have worked out well for you all and hope that they continue to do so.
Thank you – I hadn’t really heard of it either before Jessica was diagnosed. The last three years have been quite a learning curve but it is lovely to see how well she is doing now 🙂
I have never heard of Jessica’s condition before I am so happy that it all went ok and she is growing up beautifully. Look at that smile and baking! Amazing. technology really does blow me away with what we can do to save and help those in need. Thanks for linking up to Share With Me. I hope to see you again soon. #sharewithme
Thanks Jenny – the skills of the surgeons and medical technology is amazing. We are very blessed to have access to such wonderful healthcare and it is such a joy to watch her grow and develop. Lovely to link up with you again 🙂
The wonders of modern medicine are the lives it saves are awe inspiring x #sharewithme
Thank you – yes am very grateful for modern medicine and the miracles it can perform 🙂
Wow, this is amazing, and a testetment to your little girls, you and your families strength. She is a little darling!
Thank you – she is a wonderful little girl and we are very blessed 🙂
What a fascinating and amazing story which I am so glad you shared. I had never heard of this before. Bless your daughter, she is beautiful and sounds like a real survivor. You are one amazing Mum too. Thank you for linking to PoCoLo 🙂 x
Thanks Victoria – she certainly is a little survivor. Lovely to link up with PoCoLo 🙂
I can’t imagine the thoughts you live with on a daily basis, so glad Jessica is happy and well, I wish you all well for the future whatever it may bring. #pocolo
Thank you 🙂
This must have been so difficult and I can’t get over how strong you must have been. Those pictures of her are so sad bless her. I’m so glad she is doing so well and I think by reading this blog you definitely make the most of every second!! Lots love xx #thetruthabout
Thanks Sarah – it has been a difficult journey but there have been many moments of joy along the way too and looking back definitely makes me realise how very lucky we are x
Great explanations of the biology of it all hon. You really have had to deal with so much and so has Jessica in her short life. She’s a toughy! Modern medicine is amazing isn’t it? Love her happy little face helping with the baking 🙂 Thanks so much for linking up to #thetruthabout Xx
Thank you Sam, she certainly is a tough cookie and modern medicine is an amazing thing. Lovely to link up to #thetruthabout again x
I loved reading all the posts on your page. I know your road somewhat well. My 6 year old is a hypoplastic right heart. I was glad to see her pictures and how wonderful she looks. She’s a beautiful little girl. Not too many people understand what it’s like to be a heart mommy and all the things that come with it. So I wanted to wish you and your family all the best and let you know how much your posts mean to some people.
Thank you for your lovely comments Bethany and so glad that you liked my posts. Hope your daughter is currently doing well x