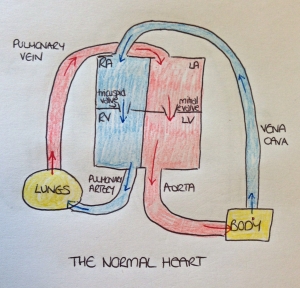
My eldest daughter Jessica was born with a congenital heart defect called hypoplastic left heart syndrome. This is my basic understanding of how Jessica’s heart worked, although firstly I need to explain how the normal heart works. The picture below is a very simplified diagram representing the normal circulation. In the normal heart, oxygen-rich, or oxygenated, blood enters the left atrium of the heart via the pulmonary vein. It is pumped through the mitral valve into the left ventricle and then pumped into the aorta where it travels to the body. The blood leaving the body is known as deoxygenated blood (the oxygen having been used by the body) and this returns to the right side of the heart via the vena cava, entering the right atrium where it is pumped via the tricuspid valve into the right ventricle. It is then pumped from the right ventricle into the pulmonary artery where it travels to the lungs to collect oxygen. The oxygenated blood now leaves the lungs via the pulmonary vein and travels back to the heart and the process begins again.
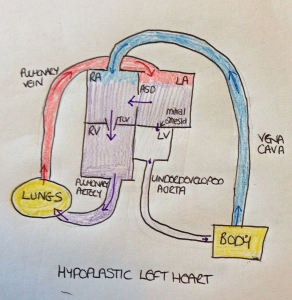
With hypoplastic left heart, the mitral valve is blocked (known as mitral atresia) which prevents the oxygenated blood getting to the left ventricle. However, an atrial septal defect (ASD) (a hole between the top two chambers of the heart) usually forms to allow the blood from the left atrium to pass into the right atrium where it mixes with the deoxygenated blood before passing into the right ventricle, through the pulmonary artery and back to the lungs. Because very little blood is able to get into the left ventricle and into the aorta, the aorta is underdeveloped.
Whilst the baby is in the womb, there is a duct known as the ductus arteriosus connecting the pulmonary artery and the aorta and this allows blood to pass into the aorta and on to the body. However, this closes a few days after birth and so unless surgery is performed, the baby will die.
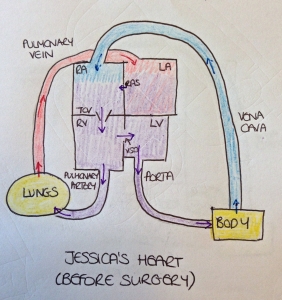
In Jessica’s case, there was an added complication known as a restrictive atrial septum, which meant that the hole connecting the top two chambers of her heart was very small and was quite likely to close soon after birth. Before birth this was less of a concern because in the womb, there is a hole between the atria, known as the foramen ovale, which allows blood to travel between the top two chambers. Again this closes very soon after birth and so in Jessica’s case, this would have meant there was nowhere for the blood to go once it entered the left atrium. She also had a ventricular septal defect (VSD) which is a hole between the bottom two chambers which allowed some blood to pass into the left ventricle and out through the aorta so her left ventricle was not quite as underdeveloped as in many cases of hypoplastic left heart syndrome.
Because of her restrictive atrial septum, Jessica’s prognosis was particularly poor and we were very lucky to be offered fetal surgery to enlarge her atrial septal defect and improve the blood flow between the top two chambers of the heart. After she was born, she needed a further procedure to widen this hole once more and to create a stent between her aorta and pulmonary artery, effectively recreating the fetal circulation in order to allow her time to grow before her next heart surgery.
Jessica’s heart could not be fixed but through a series of operations, the surgical team re-plumbed the blood vessels around her heart so that the right side of her heart did all the work (meaning that she effectively had half a working heart). The blood was pumped from the right ventricle around the body and then returned to the lungs under its own pressure (rather than being pumped back through the heart) where it collected oxygen and then returned to the heart before being pumped back around the body. This was done as a series of three operations known as the Norwood procedure, Glenn procedure and Fontan procedure. Jessica had her Norwood and Glenn procedures (plus two operations known collectively as the hybrid procedure prior to her Norwood) and her Fontan procedure was carried out in December 2017.
About thirty years ago, there was no treatment (other than heart transplant) for hypoplastic left heart syndrome and so life expectancy is unknown. We were told when Jessica was first diagnosed at the 20 week scan, that there was a 50% chance of her living to the age of five and if she made it that far, she would have a good chance of living into her teens and early adulthood. Beyond that, we didn’t know. Later, when it became apparent that Jessica’s anatomy was more complex, we were told that she was unlikely to be suitable for surgery at all and that compassionate care (making her comfortable until she passed away) would be offered instead (we had declined the third option of termination). We are hugely grateful for being given the chance for fetal surgery which gave Jessica the option of post-birth surgery and helped us to have the time we had with her.
Jessica’s future was always uncertain and we lived day-to-day, enjoying the moments and trying not to let the fear of the future rob us of the joy we had with her. Sadly, Jessica became unwell with a series of viruses a few months after her Fontan, and died unexpectedly on 14 April 2018.
Living life without our beautiful big girl is the hardest thing we have ever had to do. We are so thankful for the time we had with her though. We were blessed with six and a half years. It was longer than we’d dreamed we’d have in those early days, but we will always wish we could have had longer. Jessica brought us so much joy throughout her life. She was our little miracle and we will always be proud to be her parents.


Only getting to read this now, such an amazing little girl you have and what a journey ye are on. It’s truly amazing what modern medicine can do and a little hope and faith, I truly hope your little girl will continue to enjoy life and thrive for many many many years to come xxx
Thank you – she is a little fighter bless her and we are very thankful for the wonders of modern medicine and all the love and prayers that have supported us so far xx