A few weeks ago, I was contacted by Action Medical Research, a charity which funds medical research on children’s disease. They wanted to use a photo of Jessica in their supporter magazine to highlight the research that they are jointly funding with Great Ormond Street Hospital Children’s Charity into improving surgery for babies born with hypoplastic left heart syndrome (HLHS). As a mother of a child who has HLHS, I was quite interested to read more about this research.
Hypoplastic left heart syndrome is a complex congenital heart defect where the left side of the heart is severely underdeveloped. Without surgery, babies born with HLHS will die shortly after birth. In order for children born with HLHS to be able to survive into adulthood, they will need to undergo at least three complex heart surgeries. These surgeries basically “replumb” the heart to allow the right side of the heart to do all the work, effectively meaning that people who have HLHS effectively live their lives with half a working heart.
35 years ago, the first successful surgery took place on a baby with HLHS – the Norwood procedure, named after Dr William Norwood, who pioneered this surgery. The Norwood procedure is usually the first surgery that a baby with HLHS undergoes, normally being performed before the baby is a couple of weeks’ old. However, for some babies, like Jessica, a different surgery may be performed before, or instead of, the Norwood. In Jessica’s case, her particular anatomy meant that she was higher-risk for the Norwood procedure and so she had a procedure called the hybrid procedure to give her time to grow, and her Norwood procedure took place when she was three months old.
Each child’s heart anatomy is different. The surgeries for HLHS are high-risk and complicated, and sadly some children will not survive the procedure, whilst others may have ongoing health problems resulting from surgery. It can be difficult to know exactly which surgical technique may be best for each individual child and there is very little evidence on the pros and cons of each.
The research that is being funded by Action Medical Research focuses on using analysis of MRI scans of more than 150 babies with HLHS to produce computer-generated 3D models of each child’s heart and the main blood vessel going to the body – the aorta. They can then compare models of the child’s heart before and after surgery, looking at the blood flow through the heart and aorta to analyse the benefits and drawbacks of different surgical techniques. This will help surgical teams to plan treatment options for babies born with HLHS and therefore hopefully will improve outcomes for them.
To find out more about Action Medical Research and this research, please click here.
I have written this post to help raise awareness of this research as part of a series of posts for Heart Week 2016. This is a cause which is very close to my heart and I have not been compensated in any way for writing and sharing this post. Action Medical Research is a registered charity (charity no. 208701)

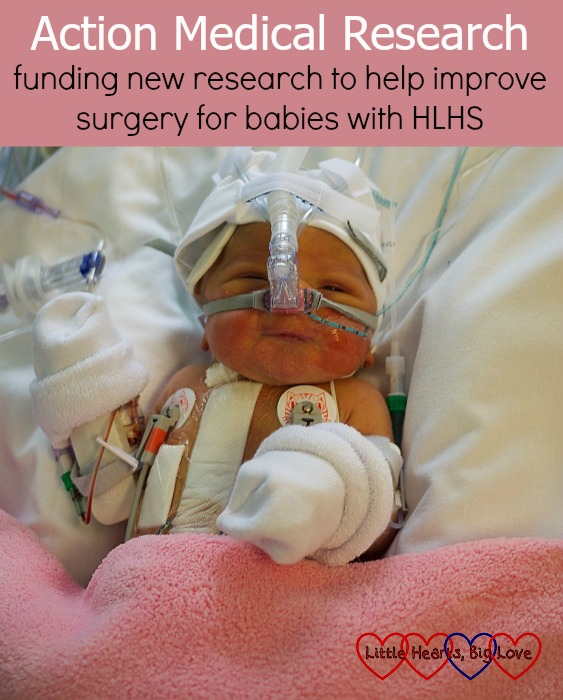
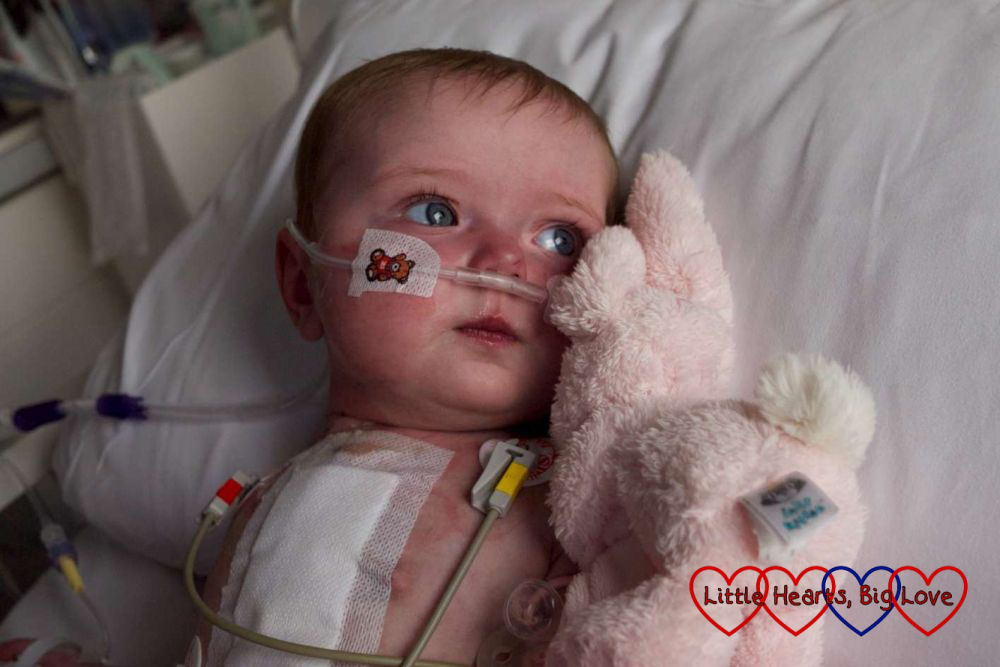

Those photos bring tears to my eyes – how hard it must have been got you then but how wonderful to see the photos of her now on the blog, years on. It’s a great cause to support and I hope the research can help many more babies. #bloggerclubuk
Thank you Cathy – the research sounds amazing and hopefully will help improve the outcomes for HLHS babies undergoing surgery in the future.
What a great cause! The research sounds amazing x
It does sounds amazing – hopefully it will help more babies to get through surgery x
An amazing charity…so important to do this research and learn more about the condition. It must have been so hard for you to go through at the time but seeing her now is just brilliant. Modern medicine is incredible #bloggerclubuk
Thank you Elizabeth, modern medicine is amazing – I am in awe of what can be done these days through computer modelling and 3D printing.
I can not imagine what you and your hubby went through throughout the pregnancy and Jessicass first years and what you continue to go through now. The research sounds fantastic and hopefully will be able to save other babies lives. Great post to raise awareness. Thank you for joining us at #BloggerClubUK hope to see you again next week X
It’s certainly been quite a rollercoaster! I found it so interesting to read more about the research – it’s amazing what can be done with technology now and hopefully it will help to improve outcomes for other babies.